Unlocking the Power of Medical Coding:
In the complex world of healthcare, medical coding plays a crucial role in ensuring accurate billing, proper reimbursement, and compliance with industry standards. Whether you’re a healthcare provider or a medical billing professional, understanding the fundamentals of medical coding is essential to streamline operations and maintain financial health.
What is Medical Coding?
Medical coding is the process of translating medical diagnoses, procedures, and services into universal codes that insurance companies and other healthcare organizations use to process claims. These codes ensure that the correct procedures and services are billed and that payments are made promptly.
Medical coding relies on a set of codes and classification systems, including ICD-10 (International Classification of Diseases), CPT (Current Procedural Terminology), and HCPCS (Healthcare Common Procedure Coding System). These codes provide a standard language for the medical community to ensure uniformity and reduce confusion when describing medical treatments, diagnoses, and procedures.
![]()
The Importance of Medical Coding in Healthcare
Accurate medical coding is crucial for several reasons:
-
Proper Billing and Reimbursement
Proper medical coding ensures that healthcare providers are reimbursed accurately for the services they provide. Incorrect or incomplete coding can result in delayed or reduced payments, impacting the practice’s cash flow. -
Compliance with Legal and Regulatory Standards
Healthcare is one of the most regulated industries, and medical coding ensures that healthcare providers comply with various laws and regulations, such as HIPAA (Health Insurance Portability and Accountability Act). Incorrect coding can lead to legal penalties, audits, and even fraud accusations. -
Accurate Patient Records
Medical coding helps maintain accurate patient records, ensuring that the right diagnosis and treatment are documented. This is critical not only for billing purposes but also for patient care, as it allows other healthcare providers to access the patient’s medical history and make informed decisions. -
Data Analysis and Research
The data generated from medical coding is invaluable for healthcare research and analytics. By analyzing coded data, organizations can gain insights into health trends, treatment outcomes, and disease patterns, which can improve overall care delivery.
Common Challenges in Medical Coding
While medical coding is essential, it comes with its own set of challenges. Some of the most common issues in medical coding include:
-
Code Selection Errors
Medical coders must carefully select the correct code from a vast list of available options. An incorrect code can result in denied claims, delayed payments, and audits. -
Up-to-Date Knowledge
Medical coding is constantly evolving, with new codes being added and existing ones being updated regularly. Coders must stay current with these changes to ensure compliance and accurate billing. -
Complexity in Procedures
Some medical procedures are more complicated than others, requiring a deep understanding of medical terminology and procedures. Coders need extensive training to handle complex cases accurately. -
Insurance and Payer Variations
Different insurance companies and payers have varying coding requirements. Coders must understand each payer’s specific guidelines to prevent rejected claims.
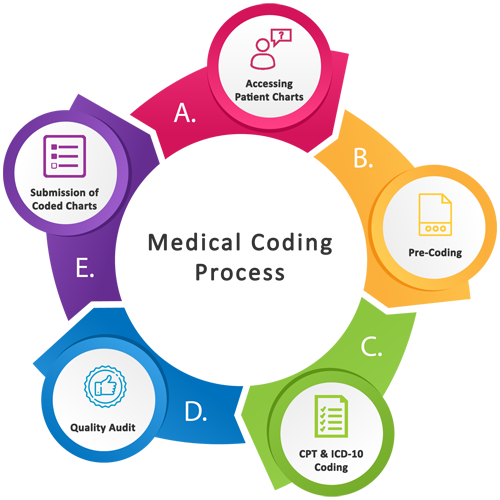
Medical Coding in the Billing Process
Medical coding is the backbone of the medical billing process. Here’s how it fits into the overall revenue cycle:
-
Patient Visit and Documentation
When a patient visits a healthcare provider, the provider documents the diagnosis and treatment. The medical coder then reviews this documentation to select the appropriate codes. -
Code Assignment
After reviewing the medical records, the coder assigns the correct ICD-10, CPT, and HCPCS codes. These codes are used to describe the patient’s diagnosis, the procedures performed, and any other services rendered during the visit. -
Claim Submission
The coded information is then used to create a claim, which is submitted to the insurance company for payment. Accurate coding ensures that the insurance company can process the claim without delays or denials. -
Payment and Reimbursement
Once the claim is approved, the healthcare provider is reimbursed for the services provided. Medical-coding ensures that the provider receives the correct payment based on the codes submitted.
The Role of Technology in Medical Coding
Technology has significantly impacted the medical-coding process, improving efficiency and accuracy. Some of the key technological advancements in medical-coding include:
-
Automated Coding Systems
Many medical billing companies and healthcare providers now use automated coding software to streamline the coding process. These systems help coders identify the correct codes quickly, reducing human error and increasing efficiency. -
Electronic Health Records (EHRs)
EHRs have transformed how patient data is documented and accessed. EHR systems integrate medical-coding, allowing coders to quickly select and apply the correct codes based on the patient’s visit. -
Artificial Intelligence (AI) and Machine Learning
AI and machine learning algorithms are being used to predict and suggest the correct codes based on patterns in the data. This helps reduce the time spent on coding and minimizes errors. -
Cloud-Based Solutions
Cloud-based medical coding platforms allow coders to access the most up-to-date code sets, collaborate with other team members, and manage coding workflows more efficiently.
How to Improve Medical-Coding Accuracy
Accurate medical-coding is essential for effective billing and reimbursement. Here are some tips to improve coding accuracy:
-
Ongoing Training and Education
Medical-coding is a constantly evolving field, so it’s crucial to invest in regular training and professional development for your coding team. This ensures they stay up-to-date with the latest code changes and industry best practices. -
Implement Quality Control Checks
Implementing a system for double-checking codes before submitting claims can reduce errors. Having multiple layers of review ensures that mistakes are caught before they affect the billing process. -
Use Up-to-Date Coding Systems
Ensure that your coding team uses the most current version of ICD-10, CPT, and HCPCS codes. Outdated code sets can lead to inaccuracies and reimbursement issues. -
Encourage Collaboration Between Coders and Healthcare Providers
Effective communication between coders and healthcare providers is essential. Coders should have access to comprehensive medical records and consult with providers when unclear about a diagnosis or procedure.
Conclusion
Medical coding is a vital aspect of the healthcare billing process. By ensuring accurate coding, healthcare providers can improve reimbursement rates, avoid legal issues, and maintain accurate patient records. The evolving nature of medical-coding demands constant training, attention to detail, and the use of advanced technology.
For healthcare providers and medical billing companies, staying informed about the latest developments in medical-coding is essential for success. By implementing best practices, investing in technology, and ensuring continuous education for coders, you can streamline the billing process and improve your practice’s revenue cycle.
![]()
By focusing on medical-coding, healthcare providers and billing companies can unlock the full potential of their revenue cycle management. For more information about how accurate coding can benefit your practice, contact Icon Billing LLC today!